Regional anesthesia is a powerful tool in perioperative care and pain management, with significant research driving technical and technological improvements. However, clinicians in resource-limited settings may not have access to medications or equipment that form the gold standard in resource-rich settings. They may also commonly face shortages of anesthesiologists, limited access to advanced monitoring, unreliable electricity, and constrained supplies of medications. Innovation in regional anesthesia techniques has helped to combat disparities between these environments, with clinicians employing strategies to provide the best care possible despite constrained resources.
Regional anesthesia, broadly defined as techniques that block sensation to a specific part of the body, offers several intrinsic advantages in resource-limited environments. It reduces dependence on airway equipment, anesthetic gases, and ventilators, which may be scarce or too expensive. Additionally, patients remain able to breathe spontaneously, which often necessitates less intensive monitoring and postoperative care. These features are useful in places where healthcare infrastructure is limited but surgical need is high.
Innovation in these settings is rarely driven by cutting-edge technology alone. Instead, it often reflects thoughtful reengineering of existing methods. Landmark-based nerve blocks, which have been replaced with ultrasound-guided blocks in many well-equipped facilities, remain very useful when ultrasound machines are unavailable. Clinicians have refined these approaches through deep anatomical knowledge, careful patient selection, and accumulated experience. In some regions, modified spinal and epidural techniques using lower doses of local anesthetics have been developed to minimize hypotension in patients who may be malnourished or volume depleted.
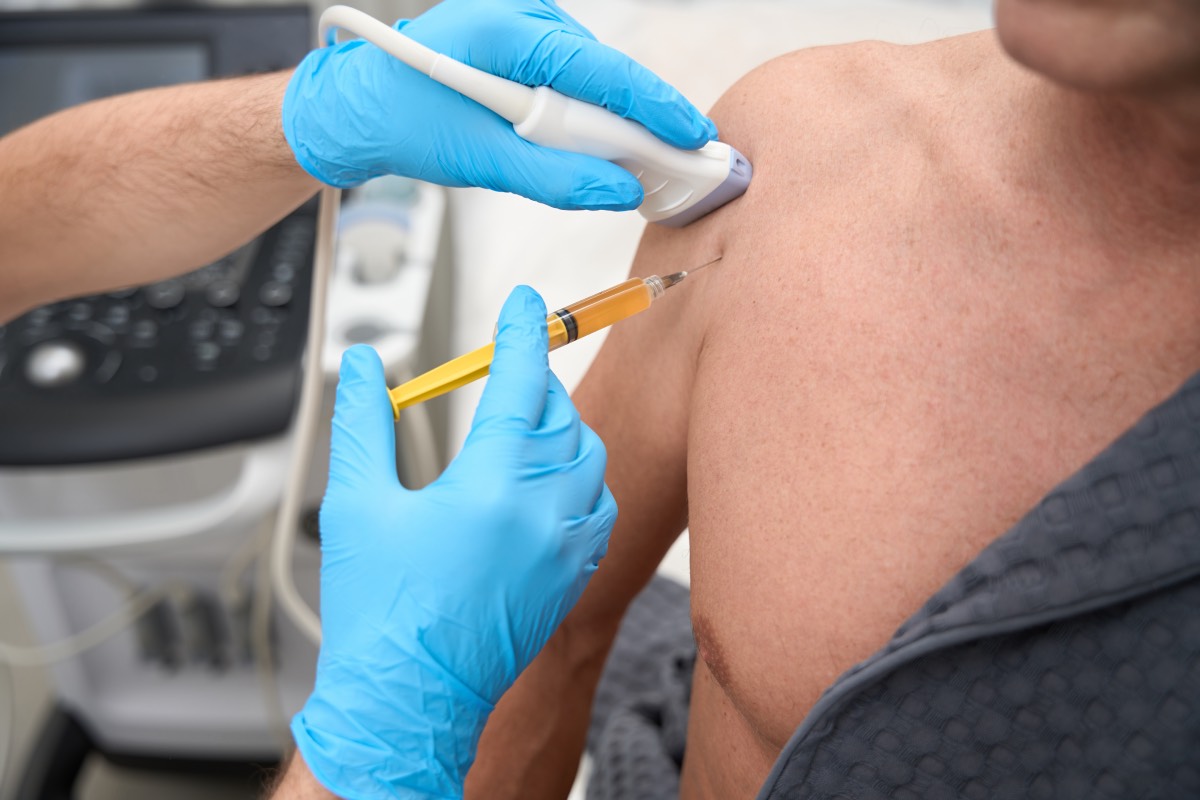
At the same time, technological advances have begun to reach even constrained environments in adapted forms. Portable, battery-powered ultrasound devices are increasingly being introduced to resource-limited healthcare settings through global health partnerships. When combined with targeted training programs, these devices have transformed the safety and precision of regional anesthesia, even in small hospitals. Innovation here lies not only in the device itself, but in how it is integrated into practice, shared among departments—potentially supporting regional anesthesia, point-of-care ultrasound, and obstetric care—and maintained under challenging conditions.
Education and task-sharing represent another branch of innovation in regional anesthesia in resource-limited settings. When physician anesthesiologists are few, non-physician anesthesia providers often deliver the majority of care. Structured training in regional anesthesia has allowed these providers to safely expand their scope of practice, improving surgical access while maintaining acceptable safety profiles. Simulation using low-cost models, peer-to-peer teaching, and context-specific guidelines have proven more impactful than importing protocols designed for vastly different healthcare systems.
Drug availability also drives creative adaptation. Limited formularies have prompted renewed interest in longer-acting local anesthetics and adjuvant techniques that prolong block duration without increasing cost. The careful reuse of multi-dose vials under strict infection-control practices, while controversial, reflects the ethical tension between ideal standards and real-world constraints.
Importantly, innovation in regional anesthesia within resource-limited settings should not be viewed as a temporary substitute for “ideal” care. Many of the approaches developed under constraint offer lessons for global anesthesia practice, including simplicity of technique, judicious use of resources, and patient-centered decision-making. As global surgery initiatives expand, there is increasing recognition that innovation flows in multiple directions, and that high-income systems have much to learn from clinicians who deliver effective anesthesia with minimal tools.